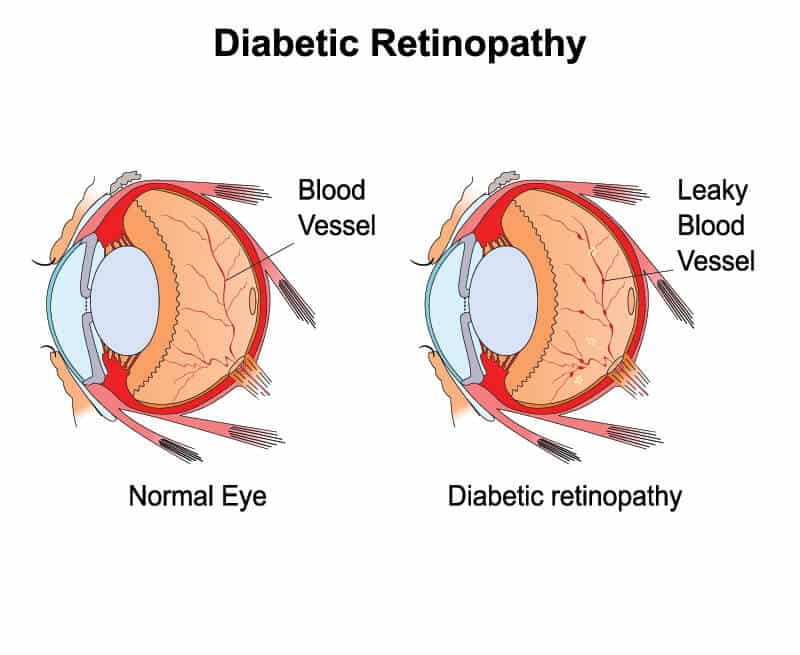
Patients with diabetes can develop damage to blood vessels in the retina over time. This damage is called diabetic retinopathy. Damage due to diabetic retinopathy can lead to vision loss if not diagnosed and treated properly. In fact, diabetic retinopathy is the leading cause of new cases of blindness in adults in the United States. Patients with diabetes require regular dilated eye examinations in order to monitor and treat diabetic retinopathy. Diabetic retinopathy can manifest in different ways.
NPDR is an earlier stage of diabetic retinopathy in which there can be spots of blood noted in the retina as well as leakage from blood vessels in the center of the retina, the macula. Leakage from blood vessels in the macula can cause swelling, called macular edema. Macular edema is a common cause of vision loss in patients with diabetes.
PDR is a more advanced stage of diabetic retinopathy in which abnormal newly formed blood vessels grow on the surface of the retina. These new blood vessels are more fragile than our normal blood vessels and they can bleed. Bleeding into the space in front of the retina, the vitreous, can occur, and is called vitreous hemorrhage. Patients with this type of bleeding often notice new “floaters” and blurred vision.
Scar tissue can grow along with these new blood vessels which can lead to a retinal detachment and can cause vision loss.
Finally, new blood vessels can form in the front of the eye, on the iris, leading to elevated pressure within the eye. Elevated pressure in the eye can lead to a form of glaucoma called neovascular glaucoma, which can be difficult to control and can lead to vision loss or blindness.
Diabetic retinopathy may have no symptoms in earlier stages and can even have no symptoms into later stages when there is advanced damage. This is why regular screening dilated examinations of the retina are important in all patients with diabetes. However, diabetic retinopathy may cause blurring of the center of the vision, usually when there is macular edema. In addition, other symptoms can include new onset floaters in the visual field with or without vision loss when there is vitreous hemorrhage. Retinal detachment may cause new onset floaters, flashing lights, and/or blurring or a shade or curtain in the visual field. Finally, neovascular glaucoma may cause vision loss, redness of the eye, and pain.
Diabetic retinopathy is caused by elevated blood sugars, typically for many years, leading to damage of the blood vessels in the retina.
Diabetic macular edema, if mild, may not need to be treated. However, significant macular edema can be treated with injections of medication into the eye and sometimes laser.
Vitreous hemorrhage can be treated with injections into the eye, and sometimes laser or vitrectomy surgery. Vitrectomy surgery is a surgical procedure in which the vitreous jelly is removed from the eye.
Retinal detachment due to diabetes may require vitrectomy surgery.
Finally, neovascular glaucoma can be treated with injections of medicine into the eye, laser, and sometimes vitrectomy surgery and/or glaucoma surgery.
Wheaton Eye Clinic retina specialists have extensive experience diagnosing and treating diabetic retinopathy. Your Wheaton Eye Clinic retina specialist will discuss with you the best approach to managing your diabetic retinopathy.
Wheaton Eye Clinic’s unparalleled commitment to excellence is evident in our continued growth. Today we provide world-class medical and surgical care to patients in six suburban locations—Wheaton, Naperville, Hinsdale, Plainfield, St. Charles, and Bartlett.
(630) 668-8250 (800) 637-1054